THIS ARTICLE/PRESS RELEASE IS PAID FOR AND PRESENTED BY SINTEF - read more
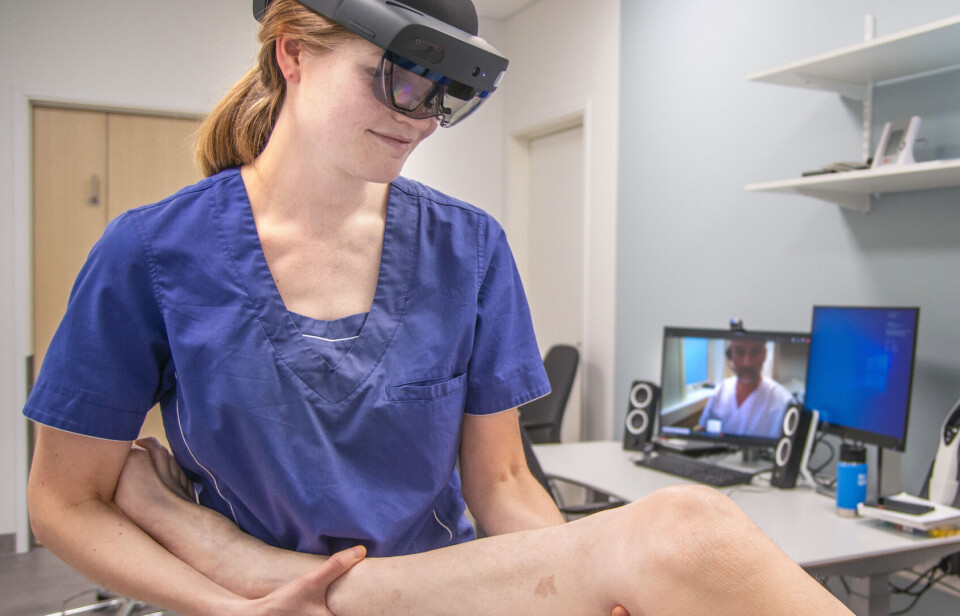
Augmented reality can be used to treat patients who live far from healthcare providers
Researchers are now making this possible with the help of local ‘health rooms’ and so-called ‘augmented reality’. Results from their experiments have so far proved to be quite promising.
Research is revealing that some patients living far away from specialist health service providers choose not to use these services because of the long distances they have to travel.
Municipal health services and hospitals in Helgeland, Northern Norway, are joining forces with a research team to find out how they can work together to alleviate the situation.
“Our aim is to move the health services closer to where people live. We’ll achieve this by testing out an entirely new addition to health service providers that we call a ‘health room’,” SINTEF researchers Kari Sand and Merete Rørvik say.
One of the key elements of the new system is Microsoft’s HoloLens headset technology, which employs a combination of augmented reality (AR) and mixed reality (MR) to enable a remote health worker to ‘see’ through the eyes of a colleague wearing the headset.
Local ‘hospitals’ with HoloLens headsets
A health room might be a real room located somewhere in the local community, such as a GP surgery, care home or other municipal facility.
“The idea is that it will contain medical equipment and technology that offer patients, next-of-kin, municipal health workers and the specialist health services new ways of interacting, as well as flexible systems enabling access to expertise and equipment,” Sand says.
The researchers are in the process of running a pilot project in Rødøy municipality in Nordland to test how the system works. They will be experimenting with services such as consultations using the HoloLens headsets.
Rørvik says that, as an example, they will see if an orthopedist at Helgeland Hospital can examine a patient with an open fracture in Rødøy with the assistance of a local physiotherapist or GP.
Less unnecessary travel
The need to develop this kind of service is the result of Norwegian geography. The sparsely populated areas and island communities of the Helgeland region are a good example.
“The health room service will be available to all ages, but will be all the more welcome to the elderly and chronically sick, who will no longer have to spend a whole day travelling for minor examinations and follow-up consultations,” Sand says.
According to Rørvik, the most important function of a health room will be to prevent patients from having to spend a great deal of time travelling to so-called ‘ten-minute’ consultations when they can get the same service locally.
“However, if you have to undergo a major operation, of course you will still have to be admitted to hospital,” she adds.
There are also indications that a health room will mean that fewer patients will have to be admitted to hospital simply ‘to be on the safe side'.
Multiple services
It is important to restructure the health service in a way that ensures that patients have equal access to care, whether they live in an island community, or just a stone’s throw from a municipal centre or a university hospital, Sand argues.
Participants in the research project have submitted many ideas about the services they want to see tested in the health room.
“They include everything from psychiatry and chemotherapy, to neurological examinations and the treatment of skin problems and open fractures,” Sand says. "We envisage that the rooms will offer scanners and x-ray machines, as well as blood transfusion equipment."
A new health service
During the project period, the health room model will be tested out on different patient groups and for a variety of clinical pathways.
“The insights we obtain will be used to make a new service model that incorporates systems that govern aspects such as funding and personnel responsibilities,” Rørvik says.
She also emphasises that the project is not being driven by economic considerations.
“However, the health room model will not make healthcare any more expensive,” she assures us.
See more content from SINTEF:
-
How fish farm nets are cleaned affects how much microplastic is released into the ocean
-
How researchers aim to protect the power grid from the northern lights’ dark twin
-
With this change, drones can fly much farther
-
New material may help combat water scarcity
-
New breakers: From climate risk to green technology
-
Why is it difficult for AI to distinguish between the sound of excavators and seagulls?





































