THIS CONTENT IS BROUGHT TO YOU BY NTNU Norwegian University of Science and Technology - read more

A new insulin mixture could make life easier for patients with type 1 diabetes
Researchers in Norway are developing a new medicine for diabetics who need daily injections of insulin. The key is a hormone that causes the smallest blood vessels to relax on the inside.
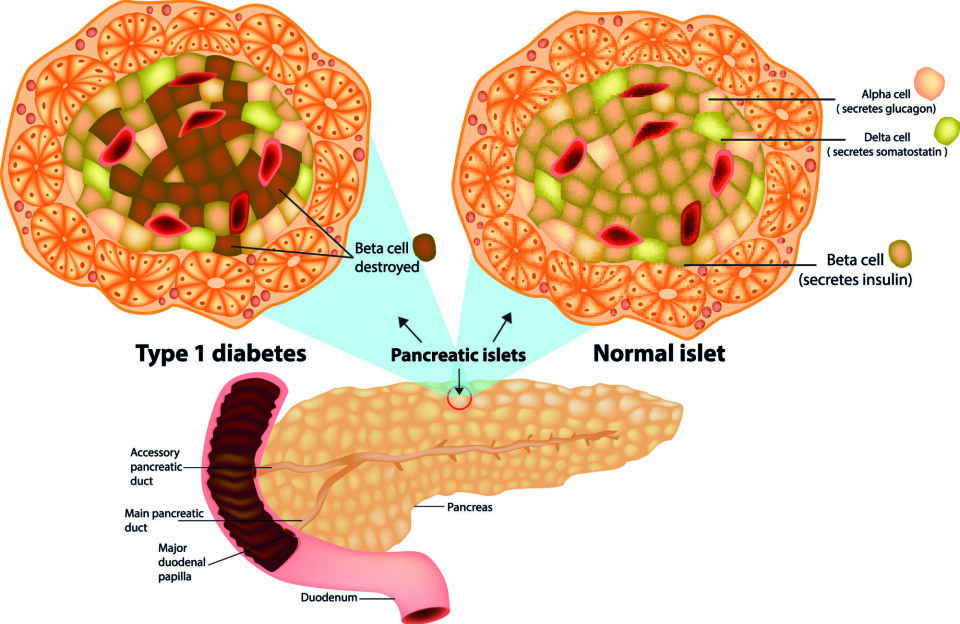
Norwegians are at the top of the list when it comes to new annual cases of type 1 diabetes among children, adolescents, and adults. This condition is caused by an insulin deficiency: the pancreas does not produce enough insulin. There is no cure, and patients must take insulin for the rest of their lives.
The Artificial Pancreas Trondheim (APT) research group has now applied for a patent for a new solution they call MicroGlucagon. It can help type 1 diabetics by inhibiting the rise in blood sugar after meals. This allows them to have better control over their blood sugar levels.
Speeds up blood flow
Insulin is needed to lower blood sugar levels. Diabetic patients lack this hormone, because their pancreas has stopped producing it. They must therefore take an accurate dose themselves, at the right time – several times a day.
This poses a fine balancing act: Too much or too little insulin can have fatal consequences.
In the new approach developed by researchers at NTNU and St. Olavs Hospital, microamounts of glucagon have been added to regular rapid-acting insulin mixtures.
Glucagon is a hormone that greatly increases blood flow in the exact area of the dermis where insulin is administered. This solution provides the body with extra assistance to quickly absorb the insulin the patient takes with their meals.
May work better and faster

“We see that MicroGlucagon can work both better and faster than the best and most effective rapid-acting insulin preparations for use with meals that are currently available on the market,” Sven Magnus Carlsen says.
He is professor emeritus, and has led the APT group since its inception in 2013. It is an interdisciplinary research group with researchers from NTNU and St. Olavs Hospital.
Promising trials involving pigs
Carlsen is an endocrinologist, an expert on organs that produce hormones and diseases that occur in these organs.
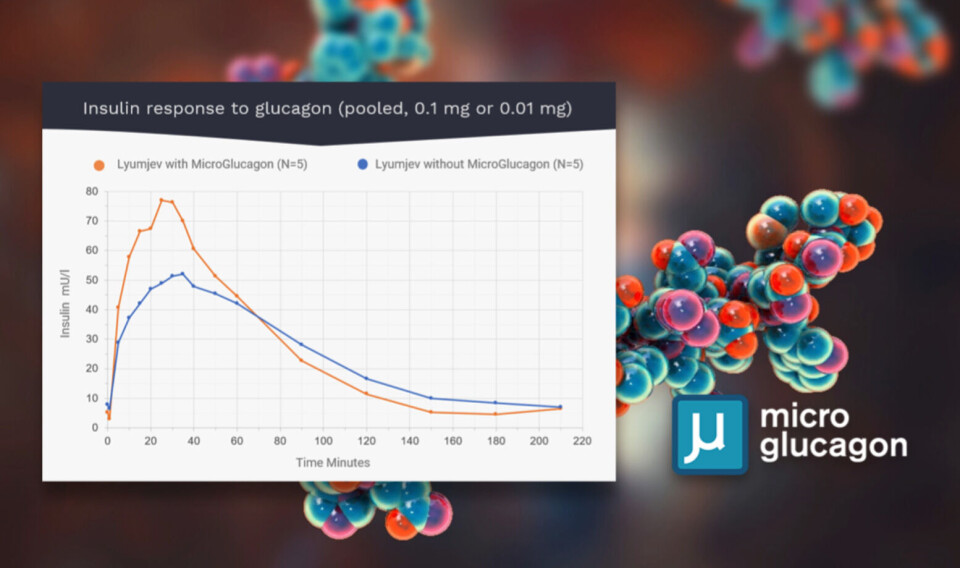
Trials carried out by the researchers on pigs under general anaesthesia show that insulin with added microdoses of glucagon reach full effect up to 10 minutes faster than the fastest insulin currently available.
Additionally, the amount of insulin absorbed by the body appears to increase when the MicroGlucagon mixture is used, perhaps by as much as 30 per cent.
Less risk of low blood sugar after consuming food
“The most important thing, however, is that when insulin is absorbed faster, it also disappears from the body faster,” Carlsen says.
The researchers believe that their solution may also reduce the risk of low blood sugar for as long as three to five hours after meals. Low blood sugar after meals can be a problem for some patients.
MicroGlucagon can be used by all patients who inject themselves with daily doses of insulin. It can also be used in insulin pumps and in semi-automatic, artificial pancreas systems.
These are so-called hybrid solutions, which are already commercially available.
If the researchers succeed in bringing the solution to the market, it will pave the way for significantly better blood sugar management in all patients with type 1 diabetes, regardless of the type of insulin treatment they use.
Goal: Fully automatic pancreas system
A lot of research and documentation remains to be done. Nevertheless, researchers can already see that the MicroGlucagon solution is helping them to achieve their goal:
“By using MicroGlucagon, we believe that the current semi-automatic solutions will improve a lot. But we also believe it will help in the development of a new, artificial, fully automatic pancreas system,” Carlsen says.
The goal is a fully automatic, closed system that constantly measures blood sugar levels. The system calculates how much insulin the body needs at any given time, and ensures that the correct doses are administered on an ongoing basis.
This means that patients will not have to constantly monitor their blood sugar levels throughout the day.

Hormone that relaxes blood vessels
Taking insulin is vital for type 1 diabetics. But it is a different hormone, glucagon, that plays the leading role in the APT group’s latest research. This hormone is also produced in the pancreas. While insulin lowers the sugar content in the blood, glucagon works to increase it.
This is how the two hormones ensure balanced glucose levels – in healthy individuals.
Glucagon has one very special property that researchers have discovered and utilised. In technical terms, the hormone causes vasodilation. This means that it relaxes the smooth muscles on the inside of the smallest blood vessels. As a result, the blood vessels expand and local blood flow increases greatly.
Minuscule doses – great effect
“What we have done, and which could be the big breakthrough, is that we have added microscopic amounts of glucagon to rapid-acting insulin solutions. In particular, we have studied the fastest acting insulin solution on the market. The point was to see if it was possible to improve what is currently the best option,” Carlsen says.
Although glucagon increases blood sugar levels, the new microdoses will be so minuscule that they will not affect the liver’s release of glucose. The risk of side effects is therefore not an issue.
In addition, adding glucagon costs almost nothing.
“We are talking about five nanograms per unit of insulin, which means that the solution contains one glucagon molecule per 420 insulin molecules. The dose is so small that the cost is negligible,” Carlsen says.
He has calculated that the annual extra cost of glucagon in Norway will be around NOK 100 (9.68 USD) for a patient with an average consumption of 60 units of insulin per day.
At the top of discouraging statistics
In total, it is estimated that around half a billion people worldwide have diabetes. The latest figures from the World Health Organization reveal that around nine million of these had type 1 diabetes in 2017.
Approximately 26,000 Norwegians currently live with this condition, and more than 400 adolescents under the age of 18 are diagnosed with type 1 diabetes every year in Norway. The number of new cases in this group has doubled every year since the 1970s, according to the Norwegian Institute of Public Health (link in Norwegian).
Type 1 diabetes cannot be prevented or avoided, while type 2 diabetes can largely be prevented through a healthy and active lifestyle.

Clinical trials will begin this spring
The researchers now have to document that the MicroGlucagon solution is stable and that it works just as effectively on humans. Professor Sven Magnus Carlsen and colleagues are preparing crucial clinical trials on type 1 diabetes patients in the spring of 2024.
Carlsen is cautious when estimating how long it will be before MicroGlucagon might hit the market. Just documenting that the solution is completely stable will take a couple of years, and drug manufacturers must also get involved.
“So, at best, it may take four to five years, but that is only if everything that remains to be done goes completely smoothly,” Carlsen says.
Seeking global actors
“Developing new medicines is a long -term race. It's both about understanding the market and the industry’s needs, and at the same time challenging solutions that already exist,” Hilde Kjeldstad Berg at NTNU Technology Transfer says.
Berg has helped the researchers with patenting and business development. The goal is to license the solution to an established industry actor during 2024.
According to Berg, it takes an average of 10-15 years before a new medicine can be launched in the market. She still thinks it can go faster with Microglucagon, since it is a naturally occurring hormone with little danger of side effects.
The world’s most technological disease
Type 1 diabetes is a complicated and challenging disease. People who get it have to self-medicate with insulin for the rest of their lives.
“Thousands of patients walk around every day treating themselves via small computers – with a medicine that, in the worst case, can actually kill them, either by not getting it, or by getting too much of it. The number of patients and the degree of technology with which they treat themselves means that type 1 diabetes is the world’s most technological disease,” Sven Magnus Carlsen.
Has to work as quickly as possible
Insulin needs to work as quickly and efficiently as possible. The time it takes is the biggest challenge. Everyone with type 1 diabetes must take rapid-acting insulin with their meals.
However, even the very fastest acting insulins on the market do not reach full effect until after an hour and a half. Patients therefore have to make sure they take insulin 15–20 minutes before eating.
“All diabetics forget to take their insulin every now and again, and even when they do remember, their meal might be delayed. Many naturally don't always know what or how much they will eat. Some people wait until after their meal to take insulin – and then it's definitely too late to achieve good blood sugar management,” Carlsen says.
Developing an insulin solution that works just as well on blood sugar when taken with a meal as it does 15 minutes before eating would therefore be a huge advance.
“The quantum leap will only take place when a fully automatic, artificial pancreas is created that provides adequate blood sugar management. We are actively working on the matter,” he says.
More content from NTNU:
-
Why seafarers have little confidence in autonomous ships
-
These house sparrows can help us save other endangered animals
-
Experienced therapists can give psychology students an extra boost
-
Teamwork is a skill – it must be practiced
-
Getting your tongue stuck: The science behind a very cold mistake
-
Why it's important that kids believe practice makes perfect





































