THIS ARTICLE/PRESS RELEASE IS PAID FOR AND PRESENTED BY the Norwegian centre for E-health research - read more

Artificial intelligence interprets your medical record
The system will automatically propose condition codes for patients' discharge summaries.
Healthcare professionals have to deal with an international system with over 30,000 codes for various diseases. It is easy to make mistakes. Researchers are now developing a computer program so that practitioners can be assisted by artificial intelligence.
Because in the healthcare system, a lot of manual and time-consuming work takes place to document a patient's care.
After each patient contact, the practitioner must write a discharge summary and record one or more condition codes that describe the type of examination or treatment the patient has received.
A discharge summary is a written summary of the examination or treatment of a patient, based on medical records.
Diagnosis becomes coded language
The person treating the patient must make a diagnosis, i.e., determine what is bothering the patient. The diagnosis must then be translated into a code based on the International Statistical Classification of Diseases and Related Health Problems, abbreviated to ICD.
In Norway, we use the 10th revision of the ICD, known as ICD-10. It is most common for the practitioner to register codes themselves, but this can also be done by office staff with special expertise.
"It takes time for practitioners to find correct diagnoses and codes. Not all information can be found in the discharge summary, so we also must look at the medical records, laboratory tests, lists of medications, and more. The patient may have been treated for a long time, and there is a lot of information that needs to be collected to be able to set diagnoses and codes," project leader in the ClinCode project, Professor Hercules Dalianis at the Norwegian Centre for E-health Research, says.

The wrong code is often recorded
The given ICD-10 codes are used for statistical purposes and to be able to predict future care needs. Researchers and clinical staff also look at the codes to quickly gain an overview of individual patient diagnoses.
Since 1997, codes have also been used as a basis for funding.
One problem with the manually set ICD-10 codes is that they are often wrong.
The ICD-10 coding system includes over 30,000 codes and can be both difficult and time-consuming to use. Often, clinicians will record the wrong codes, or will not include all appropriate codes.
An error rate of up to 20-30 per cent is estimated.
"It is important to understand that this coding tool will never be able to function optimally if the documentation that forms the basis of the coding is not good enough," Lill Irene Hind says. She is a coding adviser at the University Hospital of Northern Norway (UNN).
Incorrect and defective coding makes it difficult to bill correctly, and plan for efficient use of resources in the health service.
Computer program has learned thousands of codes
Researchers from the Norwegian Centre for E-health Research have therefore developed an automatic coding tool based on artificial intelligence that can suggest ICD-10 codes for a patient's discharge summary.
The aim of the ClinCode project is to implement a computer-supported clinical ICD-10 coding tool to improve efficiency and quality in the health service. The project is financed by the Research Council of Norway.
"The tool we call Easy-ICD is based on the fact that the program has been trained with machine learning techniques on thousands of previous patient notes and medical records in the field of gastrointestinal surgery that have already been manually coded. In this way, the program has learned which status codes a single discharge summary should receive," says Dalianis.
Gastrointestinal surgery is the surgical treatment of organs in the stomach and intestines.
Want to reduce errors
Since a large part of the training material is incorrectly coded, the system will also learn the wrong codes.
The researchers therefore want to correct the training material by recoding the data so that we reduce the errors. Easy-ICD will never be better than a human coding, but will be able to work much faster, processing huge amounts of information 24/7.
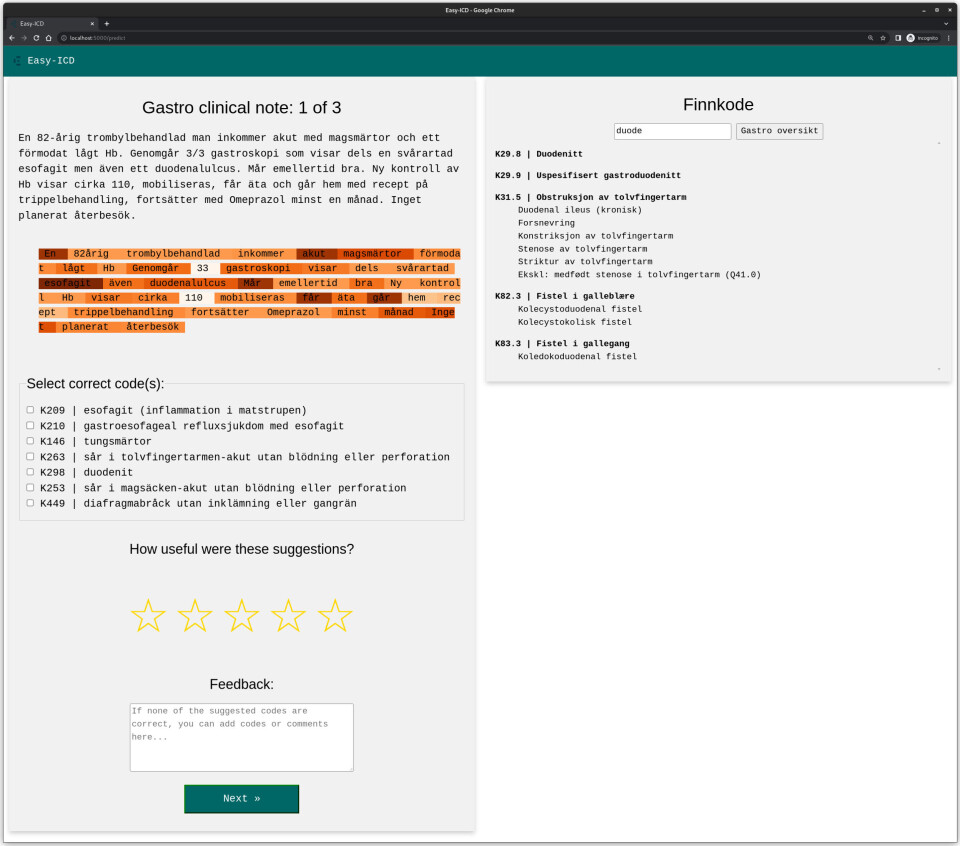
"We continue to work with Easy-ICD and work on colour-coding the important words in patient notes that lead to predicted ICD-10 codes. The colours should serve as an explanation for the user as to why Easy-ICD chose these particular codes," says Dalianis.
The idea is that Easy-ICD should propose ICD-10 codes for a specific patient, which the practitioner should be able to choose from.

This article/press release is paid for and presented by the Norwegian centre for E-health research
This content is created by the Norwegian centre for E-health research's communication staff, who use this platform to communicate science and share results from research with the public. The Norwegian centre for E-health researchis one of more than 80 owners of ScienceNorway.no. Read more here.
See more content from the Norwegian centre for E-health research:
-
When your doctor is online: People expect a reply within 24 hours
-
Technology in the health and care sector: "This is not just about new gadgets"
-
Five Nordic and Baltic countries take a major step toward the future of health research
-
A digital chatbot can help you stay fit
-
Researchers' advice for better healthcare services: Listen to the patient!
-
Half of those who received mental health care found errors in their medical records





































