This article was produced and financed by The Norwegian School of Sport Sciences
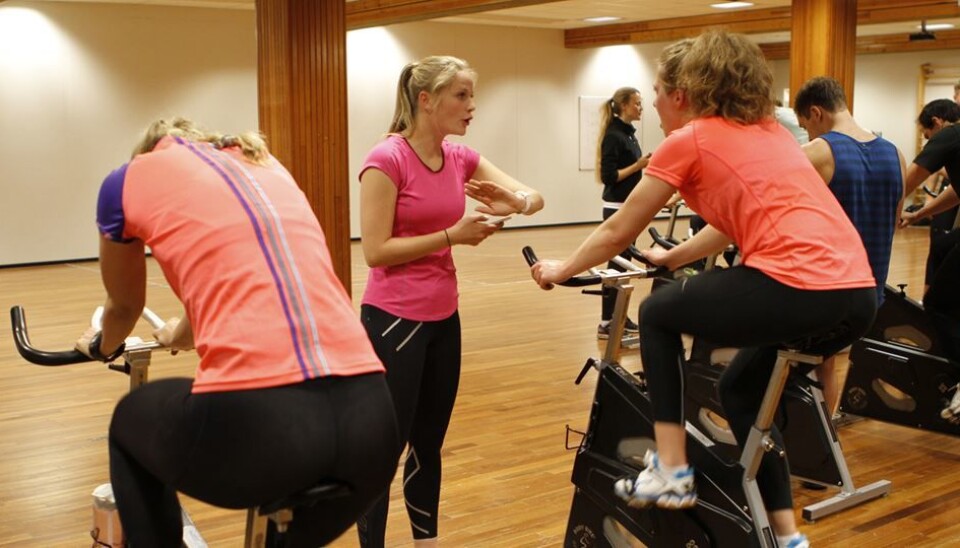
Training can treat eating disorders
New study combines training and dietary guidance as a therapy for eating disorders. Although the use of training to treat eating disorders has been controversial, the results suggest that it could be more effective than cognitive therapy.
“I thought that I would lose weight, and that was my goal when I signed up for the therapy programme. But even though I have not lost weight, I can see the value of having changed the way I think about food and exercise, which tells me it was a success.”
A quotation taken from a 28-year-old woman with an overeating disorder. She is one of 164 women with bulimia or overeating disorders who participated in the Physical Exercise and Dietary therapy (PED-t) project. The project compared the new PED-t therapy method that focuses on guided training and dietary therapy with cognitive behaviour therapy (CBT). CBT is currently the most commonly used form of therapy for eating disorders.
In the project, fifty per cent of those receiving PED-t achieved better health results, compared to the 30 per cent of participants who received CBT.
“We have to tackle the reluctance to include physical activity and training in the treatment of eating disorders. This therapy shows that it can normalise a patient’s relationship with their own body and behaviour concerning dietary and training routines,” says Therese Fostervold Mathisen, from the Norwegian School of Sport Sciences, and PhD student on the project.
Never dared to do that before
About 12 per cent of adult women have either eating disorders or disturbed eating behaviour. And 80 to 94 per cent never seek professional help. For those who contact the health services, waiting lists can be long and many find that health care personnel don't have much experience with eating disorders.
Mathisen says that they have used stricter criteria than are common to measure the improvement effect. The results shows that 29 per cent of the PED-t group recovered completely, compared to 12 per cent in the CBT group.
"There is a lot of scepticism about using exercise in therapy due to the fear of aggravating a disease that is often characterised by obsessive training to "burn calories" and curb internal turmoil,” Mathisen says.
Mathisen understands the scepticism, but based on existing literature and findings from this study, she believes that it is time to think again. The project is the first in the world that combines training and dietary guidance and compares it with the effects of CBT.
16 weeks of group therapy
The participants were randomly divided into two groups for CBT and PED-t, with a control group given no therapy during the period. Both therapy groups underwent a 16-week therapy programme in small groups.
Blood pressure, stamina, maximum strength, level of physical activity, body composition, incidence and degree of compulsory exercise, recovery from diagnosis, and reduction of symptoms of eating disorders were evaluated both before and after therapy.
“We chose to create a strength training program because it breaks with the traditional training pattern of a lot of fitness training, since many patients are keen to burn fat and calories. Strength training is also easy to do on your own, and we expected the participants to experience a feeling of empowerment,” says Mathisen.
The PED-t group were given a one-hour strength training session per week under supervision, and recieved dietary instruction. They were given exercises to do at home consisting of an hour strength training and an hour interval training, whilst the CBT group primarily had to record their thoughts and feelings on food intake.
The dropout rate was 32 per cent, with more dropping out of the CBT group compared to the PED-t group. Those who completed the therapy suffered less from depression than those who dropped out.
The effect of 16 weeks of therapy was evaluated and compared before, during, and after, and again six months and one year later. The results were stable one year after therapy, with some improvement in the CBT group.
Other things to focus on than the scales
None of the participants in the study responded negatively to training and dietary guidance. A recurring theme was that they felt more confident about food thanks to the expert guidance. Because there is so much contradictory information on food, there’s a lot of confusion surrounding what is a normal, healthy diet. It was not unusual to think that carbohydrates were dangerous.
"Instead of thinking about food as a friend or an enemy, I began to see it from a totally different angle. I think of food as nutritional components. My body needs carbohydrates to rest after exercise, proteins to rebuild muscles and cells, and fat to stimulate the brain and take care of the joints and really just to be healthy and happy," said one of the participants.
“We want to provide other things to focus on with food and exercise instead of just on calories, numbers on the bathroom scales, and burning calories by exercise. Training creates a sense of empowerment and self-confidence, which we know eating disorder sufferers score low on," says Mathisen.
Not enough physical activity and poor health
One of the unique things about this study is the monitoring of the physical health of the participants, says Mathisen. A higher proportion of participants had poorer fitness and higher levels of central obesity, which increases the risk of type 2 diabetes, cardiovascular disease, and poorer skeletal health.
“Physical health is more thoroughly evaluated in anorexia patients, because the disease is so visible and has obvious negative consequences for physical health. Our results show that health also has to be checked for patients with overeating disorders and bulimia," says Mathisen.
She also found that fewer than half complied with the health authorities' minimum recommendation for physical activity. Mathisen believes that this emphasises the need for training and dietary guidance.
More accessible therapies
One of the objectives for the project has been to find a method that is more accessible than CBT. CBT is offered only in specialist health services and certainly not by all treatment units. Then there is better access to professional training therapists and nutritionists, not least in primary health services. Training and dietary therapies can be conducted in groups, and are also more efficient for health services.
Mathisen stresses that therapists in PED-t have special skills to address this patient group's needs and considerations equivalent to a master’s degree in training and health sciences.
Her impression is that the barriers against using such a therapy programme may be lower and motivation greater.
“We use what patients themselves focus on, namely training and diet. We can lower the threshold for seeking help, many patients dread sitting down and talking to a psychologist about thoughts and feelings. Seeking help to learn how to exercise regularly and eat intelligently is more socially acceptable.
Despite the fact that there were no consultations in the training and diet programme, several participants achieved an improvement in the form of better self-esteem and increased quality of life. That confirms the results of other research that indicates that mental health problems can be improved as a direct result of proper physical exercise.
---------------
This article was originally published by the Norwegian School of Sport Sciences